Soft Tissue Sarcoma
Soft tissue sarcomas are malignant tumors that develop in soft tissue, including muscle, fibrous tissues, tendons, fat, nerves, joint tissues, and blood vessels.
Soft tissue sarcomas can occur practically anywhere in the body, although they are most prevalent in children's limbs, legs, chest, and belly.
- Soft tissue sarcomas are uncommon, accounting for fewer than 1% of new cancer cases and 3% of pediatric tumors.
- Because soft tissue sarcomas involve elastic and readily manipulated tissue, a tumor may remain undetected for a long period. During this period, it may expand and push aside the surrounding tissue.
- Soft tissue sarcomas can develop in the body for a long time without causing discomfort before being detected. Most youngsters detect a quickly growing tumor (over many weeks or months) that causes pain when touched.
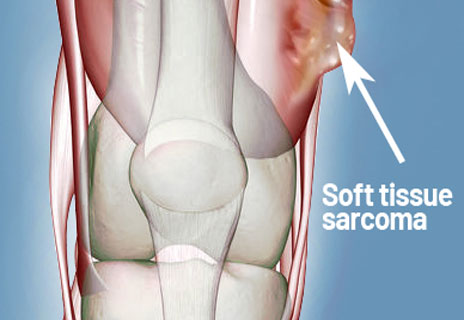
There are several forms of soft tissue sarcomas.
The most frequent are:
Rhabdomyosarcoma is the most prevalent soft tissue sarcoma in children and affects skeletal muscles.
Non-rhabdomyosarcomas may include:
- Infantile fibrosarcoma — a tumor located in the tissue that creates tendons and ligaments; this is the most common soft tissue sarcoma in newborns under one-year-old and is frequently present from birth.
- Malignant peripheral nerve sheath tumor is a tumor that forms in the cells that surround nerves and is more frequent in people with neurofibromatosis type 1.
- Synovial sarcoma is a tumor seen in tissue around joints, often the knee or ankle, but sometimes observed in the foot.
Causes of Soft Tissue Sarcomas:
The majority of soft tissue sarcomas are caused by genetic alterations that occur in tumor cells after birth. Soft tissue sarcomas have a wide range of genetic alterations, which can be discovered by testing the tumor. These alterations lead to unregulated cell proliferation and cancer genesis.
The majority of the genetic alterations associated with soft tissue sarcomas occur exclusively in tumor cells and cannot be handed down from parent to child.In rare circumstances, an elevated risk of soft tissue sarcoma has been associated with inherited genetic abnormalities, such as Li-Fraumeni syndrome or neurofibromatosis.
The most prevalent symptoms of soft tissue sarcomas are:
- Painless swelling or lump.
- Compression of nerves or muscles can cause pain and discomfort.
- Difficulty with leg and foot movement.
How are soft tissue sarcomas diagnosed?
Your healthcare professional will inquire about your medical history, symptoms, risk factors, and family history of disease. A physical examination will be performed.
You may also have one or more of the following tests:
- X-rays
- Ultrasound
- CT Scan
- Biopsy
A biopsy is the only method to confirm the malignancy.Small samples of tissue are removed and examined in a lab for cancer cells. Your findings will arrive in around a week.
After being diagnosed with soft tissue sarcoma, you will most likely require more testing. These allow your healthcare practitioners to understand more about the malignancy. They can help to determine the cancer's stage. The stage indicates how far the cancer has progressed (metastasized) in your body. It is one of the most significant factors to consider while determining how to treat cancer.
Once your cancer has been staged, your healthcare professional will discuss what this implies for your therapy.
How are soft tissue sarcomas treated?
If your kid has soft tissue sarcoma, a multidisciplinary team of healthcare specialists will care for them. Your child may see specialists such as pediatric oncologists (doctors who treat cancer in children), medical oncologists (doctors who specialize in cancer treatments), radiation oncologists (doctors who use radiotherapy to treat cancer), surgeons, nurses, social workers, rehabilitation therapists, psychologists, and other specialists.
The optimal therapy will be determined by the type of tumor, its location, the rate at which it grows, and how your kid responds to the treatment.
Most youngsters will get a mix of therapy. Options include:
- Surgical therapy involves removing all or part of the tumor.
- Chemotherapy: Anti-cancer medications are used to eliminate cancer cells. Your youngster might get a mix of medications.
- Radiotherapy uses high-energy x-rays to eliminate cancer cells.
- Targeted treatment involves using medicines that specifically target cancer cells, resulting in fewer adverse effects than chemotherapy.
- Some youngsters get hormone treatment or non-steroidal anti-inflammatory medications (NSAIDs) to prevent tumor growth.
Some children will not be treated at first, but will be constantly followed and treated if symptoms appear.
Related Treatment
A bone marrow transplant (BMT) is a therapy option for children suffering from cancer or other disorders. The purpose of bone marrow...
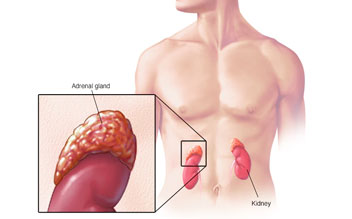
Neuroblastoma is a malignant tumor. It develops in the nervous tissue of infants and young children. Cancer cells proliferate
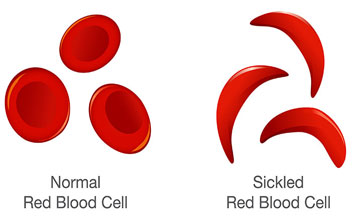
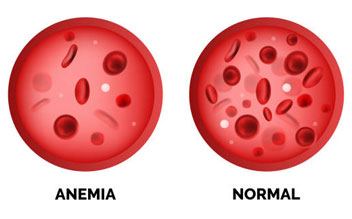
Sickle cell anemia is a hereditary disorder that affects hemoglobin, the component of red blood cells that transports oxygen...
Platelets are the cells that cause blood clots, hence platelet abnormalities cause wounded blood arteries to bleed more than usual...
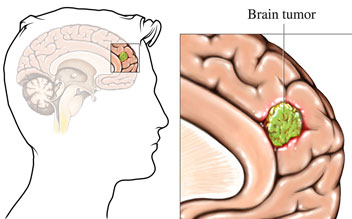
A brain tumor is an abnormal growth of tissue within the brain. The brain forms part of the central nervous system (CNS).
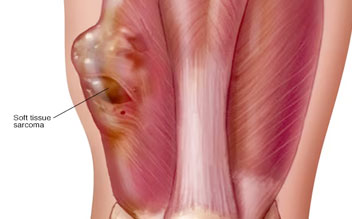
Soft tissue sarcomas are malignant tumors that develop in soft tissue, including muscle, fibrous tissues, tendons, fat, nerves,...
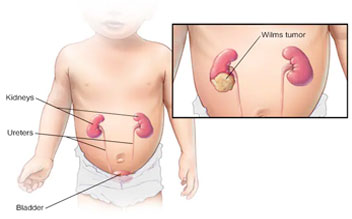
Wilm's tumor is a kidney tumor that nearly usually affects youngsters. This disease accounts for roughly 90% of kidney...
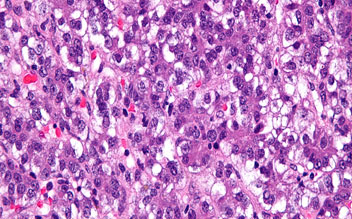
Hepatoblastoma is an extremely uncommon kind of cancer. It is a tumor that originates in the liver. It often affects children aged...
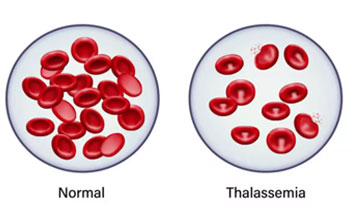
Thalassaemia is an inherited hereditary blood condition that causes permanent anemia. People with thalassaemia...