What is Neuroblastoma in children?
Neuroblastoma is a malignant tumor. It develops in the nervous tissue of infants and young children. Cancer cells proliferate in a baby's developing nerve cells while in the womb. These cells are known as Neuroblasts. It is the most frequent cancer in newborns under the age of one. It is unusual in children above the age of ten.
Neuroblastoma damages the nerve fibers in the spinal cord.
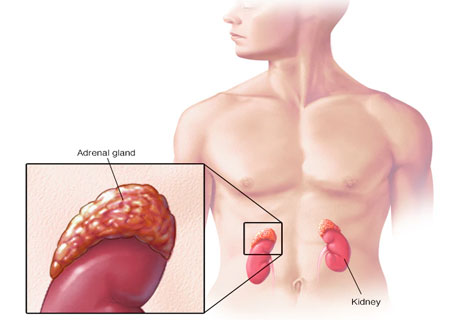
Neuroblastoma typically begins in the adrenal glands or nerve fibers in the abdomen. Other typical locations for it to develop include nerve fibers near the spine in the chest, neck, or lower belly (pelvis).
What causes neuroblastoma?
Researchers aren't sure what causes neuroblastoma.
In rare situations, neuroblastoma can run in families and be related to certain genetic problems.
The symptoms of neuroblastoma vary depending on where the neuroblastoma began and whether or not it has spread, as shown below:
- Common stomach symptoms include bloating, fullness, reduced appetite, and discomfort.
- The child may have coughing or trouble breathing if the problem originates in the chest or neck.
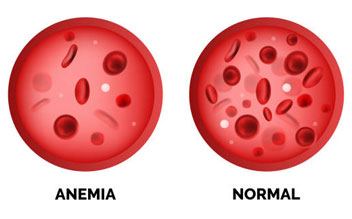
- The youngster has bone discomfort. If cancer spreads to the bone marrow, the quantity of different types of blood cells may be diminished. Anemia, or a lack of red blood cells, causes exhaustion and, in certain cases, pallor. A low platelet count produces easy bruising and little purple patches on the skin. A decrease in the number of white blood cells raises the risk of infection.
- Lumps form on the skin.
- Spread to the spinal cord: Children may experience weakness, numbness, or loss of voluntary control over certain body parts.
Less often, children exhibit signs of Horner syndrome. Horner syndrome occurs when a tumor in the neck compresses nerves on one side of the face. Children have drooping eyelids, tiny pupils, and less perspiration on one side of their faces.
Most neuroblastomas make catecholamines. Catecholamines are hormones that elevate the heart rate and produce anxiety. Other cancer-related disorders (known as paraneoplastic syndromes) include uncontrolled eye movements (opsoclonus), rapid spasms of the limbs and legs (myoclonus), watery diarrhea, and elevated blood pressure.
Testing for Neuroblastoma
If your child's doctor suspects neuroblastoma, they will undergo a series of testing. These exams are not often unpleasant. However, your youngster will need to remain motionless for some of them. Some tests may need your kid to be sleepy (sedation) or sleeping (general anesthesia).
The staff caring for your kid is used to assisting youngsters with these examinations. They will do everything they can to prepare themselves and you.
Tests for neuroblastoma may involve one or more of the following:
- Blood testing.
- Ultrasound of the abdomen
- Chest x-ray
- MRI, CT, mIBG, PET-CT, bone scan
- Bone marrow biopsy.
- Urine samples are tested.
How are neuroblastomas treated?
Treatment options vary based on factors such as tumor kind, location, growth rate, and kid response.
Some children will not be treated at first but will be constantly followed and treated if symptoms appear.
Most youngsters will get a mix of therapy.
Surgery
Surgical treatments try to remove all or part of the tumor.
Chemotherapy
Anticancer medications are used to eliminate cancer cells. Your youngster might get a mix of medications.
Radiotherapy
High-energy X-rays are utilized to eliminate cancer cells.
Bone Marrow Transplant
This is often done in conjunction with chemotherapy or radiation. It's also known as a stem cell transplant.
Immunotherapy
Some studies are being conducted on new therapies for neuroblastoma that employ the body's immune system to assault cancer cells.
Prognosis of Neuroblastoma
The prognosis relies on various factors, such as the child's age upon diagnosis, whether the tumor has spread, and specific characteristics of the tumor known as biologic features. Younger children with cancer that have not spread have the greatest prognosis.
Children with low- and intermediate-risk diseases have survival rates ranging from 90 to 95%.
The mortality rate for children with high-risk diseases was around 15%, but it has risen to more than 50% thanks to newer and more intensive techniques of combination therapy.
Related Treatment
A bone marrow transplant (BMT) is a therapy option for children suffering from cancer or other disorders. The purpose of bone marrow...
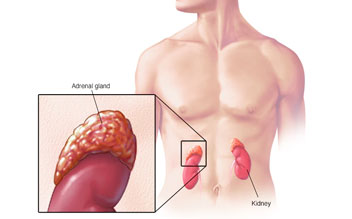
Neuroblastoma is a malignant tumor. It develops in the nervous tissue of infants and young children. Cancer cells proliferate
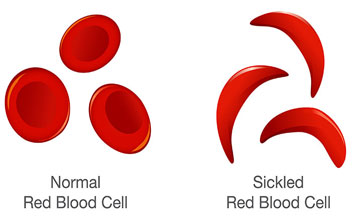
Sickle cell anemia is a hereditary disorder that affects hemoglobin, the component of red blood cells that transports oxygen...
Platelets are the cells that cause blood clots, hence platelet abnormalities cause wounded blood arteries to bleed more than usual...
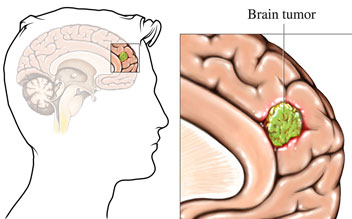
A brain tumor is an abnormal growth of tissue within the brain. The brain forms part of the central nervous system (CNS).
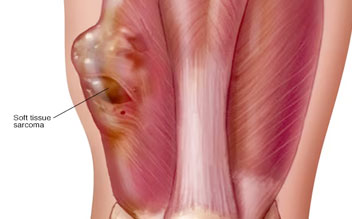
Soft tissue sarcomas are malignant tumors that develop in soft tissue, including muscle, fibrous tissues, tendons, fat, nerves,...
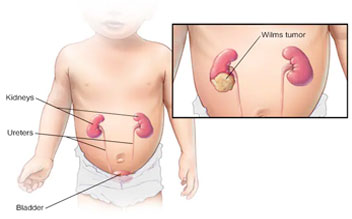
Wilm's tumor is a kidney tumor that nearly usually affects youngsters. This disease accounts for roughly 90% of kidney...
Hepatoblastoma is an extremely uncommon kind of cancer. It is a tumor that originates in the liver. It often affects children aged...
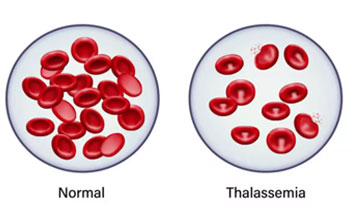
Thalassaemia is an inherited hereditary blood condition that causes permanent anemia. People with thalassaemia...